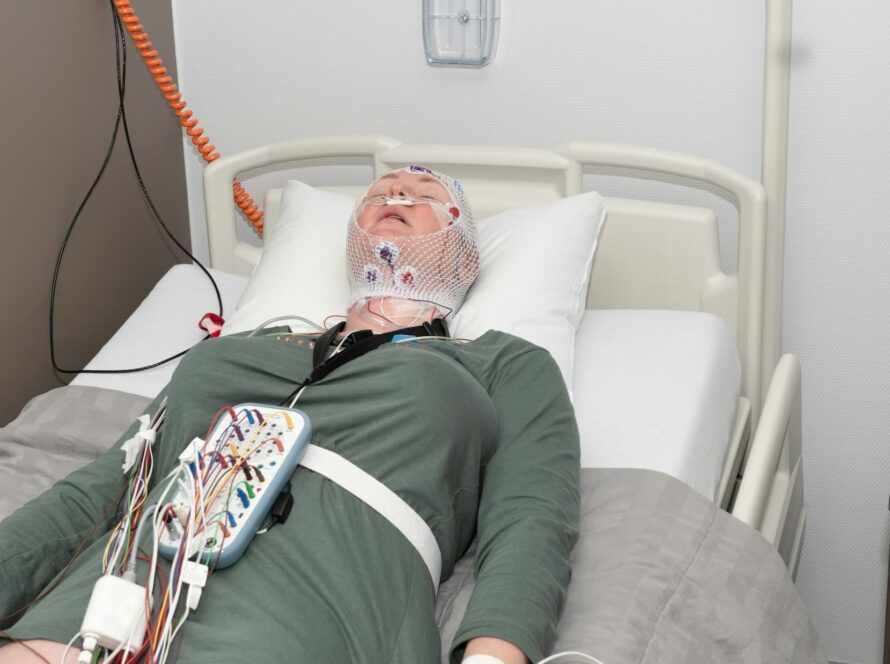
Most people think sleep problems start with obvious symptoms — loud snoring, waking up gasping, or feeling completely exhausted every morning.
But what if the root cause begins much earlier? Long before dramatic symptoms appear, subtle metabolic and hormonal changes can quietly interfere with breathing patterns and sleep stability. These internal shifts often go unnoticed, yet they can set the stage for serious sleep disorders over time.
At EL PASO SLEEP CENTER, we frequently see patients who didn’t realize their changing energy levels, mild snoring, or gradual fatigue were connected to deeper physiological changes happening at night.
Let’s talk about what’s really going on.
Your Metabolism and Your Airway Are Connected
Metabolism doesn’t just regulate weight. It influences muscle tone, inflammation levels, hormone balance, and even how your nervous system controls breathing.
When metabolic patterns shift — whether due to stress, aging, hormonal fluctuations, or lifestyle changes — they can subtly affect airway stability during sleep.
This is one reason weight and sleep apnea are often linked. It’s not just about body size; it’s about how metabolic changes influence soft tissue, muscle responsiveness, and airway control while you’re asleep.
Even small internal shifts can change how easily air flows through your airway at night.
Why Snoring Can Slowly Get Worse
Snoring rarely appears overnight. It usually develops gradually.
Many adults notice mild snoring that becomes more frequent over time. Sometimes this progression coincides with changes in stress levels, muscle tone, or metabolic efficiency — not just visible body changes.
This is why weight gain and snoring often appear connected, but the relationship is more complex than it seems. Fat distribution around the neck and throat can narrow the airway, yes — but inflammation and reduced muscle stability also play a role.
Snoring can be an early signal that airflow is becoming restricted.
It may start as a minor annoyance.
But over time, it can evolve into something more significant.
Breathing Stability Is Delicate
During sleep, your body naturally relaxes. The muscles that help keep your airway open become less active. In a stable system, breathing continues smoothly.
But if certain vulnerabilities exist, small instabilities can lead to repeated partial airway collapse.
These breathing issues during sleep may not always cause dramatic awakenings. Instead, they can create micro-disruptions — brief arousals that prevent deep restorative sleep from occurring consistently.
The result?
- Light, fragmented sleep
- Subtle oxygen fluctuations
- Increased nighttime stress response
- Morning grogginess
You may never remember waking up — but your brain was forced to.
Risk Isn’t Always Obvious
Many people assume they would “know” if they were at risk for a serious sleep condition. In reality, sleep apnea risk factors extend far beyond what most people expect.
Risk can increase due to:
- Family history
- Jaw or airway structure
- Hormonal shifts
- Chronic nasal congestion
- Insulin resistance
- Inflammatory conditions
- Stress-related muscle tension
You don’t have to fit a stereotype to experience disrupted breathing at night.
In fact, many high-functioning adults with stable careers and active lifestyles are surprised by what sleep testing reveals.
The Overlooked Impact on Sleep Health
Sleep is not just about feeling rested. It regulates nearly every system in the body. When breathing becomes unstable, overall sleep health begins to decline.
Fragmented sleep affects:
- Hormone regulation
- Blood pressure control
- Glucose metabolism
- Emotional balance
- Cognitive clarity
When restorative sleep cycles are interrupted repeatedly, the body never fully resets.
Over time, this can contribute to:
- Chronic fatigue
- Brain fog
- Reduced stress tolerance
- Slower recovery from exercise
- Mood instability
These symptoms are often misattributed to aging or a busy lifestyle.
But sometimes, the issue starts at night.
Why Many Adults Don’t Connect the Dots
One of the biggest challenges with early-stage breathing instability is subtlety.
Symptoms often build gradually:
- Slightly louder snoring
- Needing more caffeine
- Feeling mentally slower
- Mild morning headaches
- Afternoon energy crashes
Because the decline is slow, people adapt. They normalize feeling “a little tired.”
By the time exhaustion becomes undeniable, the underlying condition may have been developing for years. That’s why early evaluation matters.

What Sleep Testing Can Reveal
Modern sleep diagnostics go far beyond detecting loud snoring. Comprehensive sleep studies measure:
- Airflow patterns
- Oxygen saturation
- Brain wave activity
- Heart rate variability
- Sleep stage progression
- Micro-arousals
At EL PASO SLEEP CENTER, we often see patients shocked by how frequently their sleep is being interrupted — even though they believed they were sleeping through the night.
Objective data provides clarity. And clarity allows for targeted solutions.
Early Intervention Changes Everything
When breathing instability is addressed early, improvements can be significant and sometimes surprisingly fast.
Stabilizing airflow allows the body to:
- Enter deeper sleep stages
- Reduce nighttime stress signals
- Improve oxygen consistency
- Restore hormonal balance
Patients often report:
- Clearer mornings
- More stable energy
- Better focus
- Improved mood
- Reduced reliance on stimulants
The earlier the issue is identified, the easier it is to manage.
Listening to Subtle Signals
If your sleep doesn’t feel as restorative as it once did, or if snoring has slowly increased, it’s worth paying attention.
Sleep should not feel like something you “survive.” It should restore you.
Small internal shifts can have significant nighttime effects — and those effects can accumulate quietly over time.
Understanding the connection between metabolism, breathing stability, and sleep quality empowers you to act before symptoms become severe.
Conclusion
Sleep problems don’t always begin with dramatic warning signs. Often, they develop gradually through subtle physiological changes that affect breathing and recovery at night. Recognizing early patterns and seeking evaluation can prevent long-term health consequences and restore the restorative sleep your body depends on. When sleep works properly, everything else works better too.